Want to transform lives with us? Stay in touch and hear about our news, activities and appeals by email!
Study shows laser treatment could significantly improve treatment for glaucoma in Africa
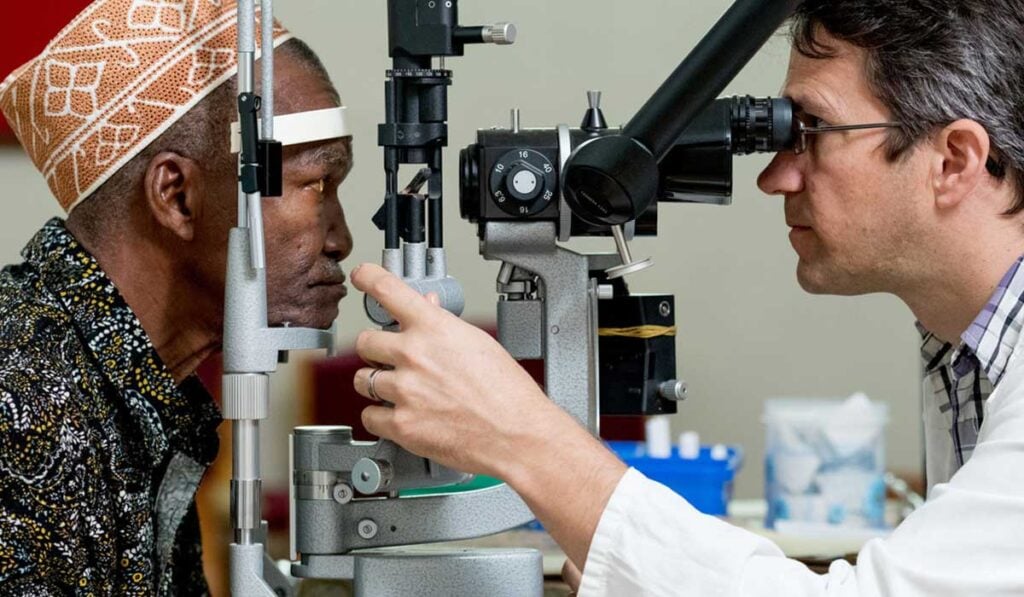
Results of a trial published in Lancet Global Health today on World Sight Day could pave the way for significant improvements in treatment for glaucoma in Sub-Saharan Africa.
The study was conducted through a research partnership between Kilimanjaro Christian Medical Centre (KCMC) in Moshi, northern Tanzania and the International Centre for Eye Health (ICEH) and was funded by CBM and Seeing is Believing (a collaboration between Standard Chartered Bank and the International Agency for the Prevention of Blindness, which concluded in 2020). It shows that laser treatment could be significantly more effective than eye drops in managing glaucoma, and can be affordable in low-income settings. The eye condition glaucoma is the second leading cause of blindness in adults worldwide. Rates in Sub-Saharan Africa are the highest for any world region and are predicted to nearly double by 2040.
The trial was led by Dr Heiko Philippin, an ophthalmologist who was based at KCMC from 2009 until 2018. He is a Clinical Research Fellow at the International Centre for Eye Health and works a glaucoma specialist at the Eye Centre of University Hospitals Freiburg. He explains:
“Glaucoma requires life-long treatment and follow up to save a person’s sight, but this is very challenging in many settings. Currently, most people are treated with eye drops but many struggle with taking them regularly or accessing new bottles, for example due to cost or distance to the nearest clinic. These study results are exciting because they show that we can treat glaucoma more successfully with a one-off or occasionally repeated outpatient laser treatment to reduce eye pressure at least for one year, compared to the most commonly used eye drops in lower income regions. We are grateful to all participants and our colleagues for their commitment and hope that these findings will improve glaucoma care for many people at risk of becoming blind.”
Kirsty Smith, Chief Executive of CBM UK, says:
“At CBM, we’re committed to building a world where nobody needlessly loses their sight. Finding innovative approaches to treating conditions like glaucoma is a vital part of that. This project has been an example of truly effective and collaborative partnership – in particular with our partner hospital KCMC in Tanzania and the inspiring research team there, and with Standard Chartered Bank and IAPB through the Seeing is Believing initiative. We’re hopeful that these exciting results will play a significant part in preventing people from becoming needlessly blind due to glaucoma in the world’s poorest places”.
This study is the first randomized controlled trial into the use of the laser treatment Selective Laser Trabeculoplasty (SLT) for patients with advanced glaucoma in Sub-Saharan Africa. It found that SLT, already widely used in high-income countries, successfully reduced eye pressure for significantly more patients in Tanzania in comparison to the standard treatment of timolol eye drops.
Glaucoma is usually caused by fluid building up in the eye, which increases intra-ocular pressure. Prompt and effective treatment is vital to prevent damage to the optic nerve and irreversible sight-loss. The treatment trial, based at KCMC, looked at effectiveness of SLT compared to timolol eye drops, currently the main treatment option in Sub-Saharan Africa.

Just, a farmer from the Kilimanjaro area of Tanzania who lives with his wife and five grandchildren, was enrolled in the trial. He started to experience sight problems more than 10 years ago and completely lost the sight in his left eye to glaucoma. This left him relying on more help from his wife and grandchildren to work on his farm. His left eye was also very painful – the pain was so severe at times that he could no longer eat. After losing the sight in one eye, Just was terrified that he might also lose sight in the other. “If I lost both sights how would I be able to go to the toilet? How would I be able to do any work?”
When he was diagnosed with glaucoma, doctors prescribed eye drops to relieve the pressure and save the sight in his right eye. Every three months, Just had to go to the clinic to pick up his medicine. It wasn’t a long trip but was still a great burden for him as it was hard to afford the bus fares and the queues were very long and hard to manage with poor sight.
After being enrolled in the trial at KCMC, Juts received laser eye treatment (SLT) on his right eye. The laser treatment worked well and reduces the burden of regular travel to pick up medication. “I am happy and I thank God because despite having low vision I have not lost sight completely”.
Dr William Makupa, Head of Ophthalmology at Kilimanjaro Christian Medical Centre, says: “In our setting glaucoma is diagnosed late, and some of the patients after sometime decide to ignore or just stop using eye drops. If we can establish an alternative effective means of arresting the disease, we would bring about a positive impact on the quality of life of these patients.”
Professor Matthew Burton, director of ICEH at the London School of Hygiene & Tropical Medicine, says:
“This result is very important for improving glaucoma treatment in low- and middle-income countries. Poor eye health has a knock-on effect across poverty, employment and development. With the number of people affected by glaucoma set to rise, studies such as these are crucial for identifying solutions that can tackle the challenge and improve the lives and livelihoods of those in Sub-Saharan Africa and beyond. Showing a significant improvement over the standard treatment for glaucoma is a real breakthrough for treating the disease in areas that historically struggle with treatment and adherence.”
How the trial worked
201 people with moderate or advanced glaucoma were enrolled in the randomized control trial. Half were treated with eye drops (timolol) and half with SLT. For those treated with eye drops, treatment was successful in 31% of eyes after one year. For those with SLT, this rose to 61%.
Where both of their eyes met trial criteria, both were included in the study – 382 eyes in total. 100 patients (191 eyes) were treated with timolol eye drops and 101 patients (191 eyes) with SLT. After 1 year, 339 eyes were analysed. Treatment was successful in 55/176 eyes treated with eye drops (31.25%) and 99/163 eyes treated with SLT (60.74%).
The study also considered the affordability of SLT, finding that in spite of the initial cost of the laser equipment, at hospitals dealing with high volumes of glaucoma patients the treatment could be offered as inexpensively as for an annual supply of eye drops. Recognizing that costs of maintaining and repairing equipment can be significant, the authors point out that the SLT laser used at KCMC has not required maintenance or repair in its four years of use.
Read the full study in the Lancet Global Health (open link in new tab).
Images: 1st – Dr Heiko Philippin carrying out laser treatment on a patient at KCMC hospital in Tanzania. 2nd – Just and his wife, standing outside their home in rural Tanzania. © CBM/Hayduk